Lyme DiseaseWhat to do if I suspect I might have Lyme DiseaseTick Bite PreventionMisdiagnosis of Lyme DiseaseHorrowitz QuestionairreUnderstanding The Causes of DiseaseThe 10 Step ProcessStep 1 - TestingStep 2 - DetoxingStep 3 - Diet and Reduction of Toxic ExposureStep 4 - Support your bodyStep 5 - Build the Immune SystemStep 6 - Support Your MindStep 7 - Kill the infectionsStep 8 - Bind the toxinsStep 9 - Control InflammationStep 10 - ExcerciseLyme DoctorsUK based Lyme Literate DoctorsNaturopathsLyme Doctors AbroadAlternative MedicineStem CellsRifeOxygen TherapyEssential OilsContact ListsBiological DentistsLive blood analysisCryotherapyIV chelationBiomagnetismIV Therapy and Vitamin InjectionsBioresonanceOzone treatment
What do I do if I have symptoms of Lyme?
If you’ve been bitten and start to feel unwell, then go to your doctor. A huge telltale sign of Lyme disease is the bullseye rash otherwise known as the Erythema Migrans rash.
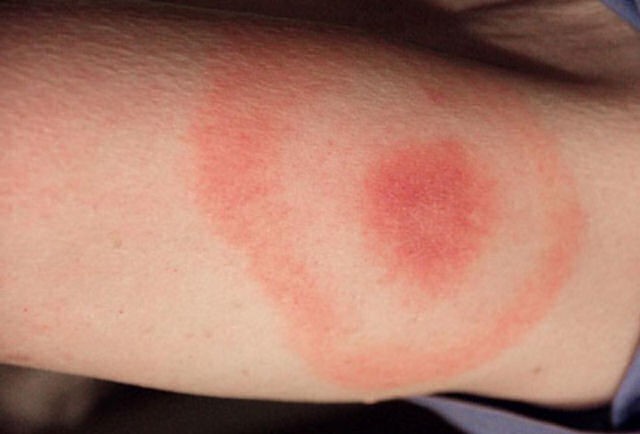
If you present with this rash the doctor should automatically dispense antibiotics. If you don’t remember being bitten and present with this rash, it’s a good indication that you have contracted Lyme. However, only 40-60% of cases with Lyme disease will develop this rash. I personally didn’t get the EM rash.
GP
When you approach your GP, he or she will perform a blood test, the Elisa, which can be an unreliable test for the reasons laid out on the previous pages. If, like me, your blood test comes back negative (which is likely if the test is taken within seven weeks of initial infection), then your GP might refuse antibiotic therapy. If your test comes back negative, then you can request that they take another blood test and ask them to send it to Porton Down (the NHS main testing facility in Salisbury, which for some reason seems to find a higher number of positives). If your GP isn’t aware that the Elisa test is quite unreliable, it can’t hurt to remind them
If your test comes back positive, you are eligible for antibiotic therapy. Below is a link to the treatment plan your GP is expected to follow.
https://www.nice.org.uk/guidance/ng95/resources/visual-summary-pdf-4792272301
The doctor will most likely prescribe you a 21 day course of doxycycline. Doxycycline is effective against early Lyme but it will only kill an active form of the bacteria and not the other two forms it mutates into in order to hide from perceived threats such as antibiotics. The most effective form of treatment they offer is IV ceftriaxone, so I would push for this if possible. It’s the most effective treatment because you aren’t consuming oral antibiotics through the digestive system, killing off good bacteria and you aren’t losing any of the potency of the antibiotic because it enters the blood stream directly.
Post Lyme syndrome
If you’ve finished your antibiotic course with the GP and you still feel unwell, this could be due to one of two things. When the bacteria die they release toxins into our body which can cause an inflammatory response. With a Lyme infection, the fluid around the cells can become sticky and sluggish. As a result, the lymphatic system plugs up, the liver slows down and toxins from dead bacteria can be left to linger in the body, being absorbed by the brain and the nerves, which can then set off various other conditions such as Parkinson’s and MS. This can usually be resolved with lots of detoxification (see our guide to detoxification). If after detoxification you are still experiencing ongoing symptoms, then the chances are the antibiotics weren’t effective and you still have an active infection. In my honest opinion and due to the stealthy nature of Lyme disease and co-infections, an ongoing infection would be the most likely answer if you are still experiencing symptoms post NHS antibiotic treatment. Respected Lyme doctors in America recommend treating Lyme two months past your last symptom but they have their patients on thorough detox regimes at the same time.
Join the LDUK support group.
This support group has been a life line to me and I recommend that any potential Lyme sufferer join. Lyme Disease is a very distressing disease and the symptoms can have a huge impact on your mental health. Not just because the disease actively depletes and disrupts the happy, positive neurotransmitters in your brain which leads to depression and anxiety but also because the loneliness of not having people understand and the feeling of being constantly unwell can be soul destroying. It’s comforting to have access to a community that understands exactly how you feel and can relate to the strange and crazy symptoms that crop up. Among the members are some of the UK’s foremost experts on Lyme disease who may not have doctorates but have years of experience and are incredibly well versed in Lyme. Most of them, like me, became unintentionally knowledgeable through necessity. The LDUK website also provides valuable information for Lyme patients.
LDUK support group
https://m.facebook.com/groups/481294698590907
LDUK website
http://lymediseaseuk.com
Infectious Disease Specialists
I and many others in the community have seen multiple infectious disease specialists and the majority of us have left their consulting rooms extremely deflated. Some have Lyme disease listed as their specialty but many of them might not be up to date with the current thinking coming from experienced Lyme doctors in the USA and Europe, where the disease has been prevalent a lot longer. They are working within a set of guidelines as to how the disease used to behave before it mutated and added various co-infections to its armoury. With new guidelines on how to treat the disease, new data that indicates that Lyme disease is now in every county in the U.K, I hope that the general attitude within the NHS infectious disease community will change. However, they are limited as to what they can provide in terms of treatment and have to operate within various guidelines. If your next port of call is to be referred to an infectious disease specialist and they insist that you don’t have an active infection, they may be right but if you are still having ongoing and new symptoms and your instinct is telling you that you are still infected, then my advice is to trust your instincts. You could be led down a path of an alternative diagnosis and waste valuable time while the infection takes further hold. It’s your body, the rest of your life and it’s 20 minutes of their day. I ignored all my infectious disease specialists and pursued with testing and treatment abroad. Which confirmed, despite what they told me that I still had Lyme and multiple co-infections. If I had let the specialists have the last word on this and continued my care with them, I believe I would be now living with a diagnosis of ME or MS. As a side note, I was recently admitted to hospital for a common complaint and the care that I received from the doctors and nurses was exceptional. However, when it comes to new and emerging strains of Lyme and co-infections, the UK has a way to go.
What Next?
So, you’ve been to see your doctor, you may have had a positive or most likely negative test for Lyme, they have given you antibiotics, maybe referred you to an infectious disease specialist and it’s at this point you have hit a brick wall. This is the time to find a Lyme specialist. These are either doctors abroad or in the U.K. that are operating privately and without the restrictions that NHS doctors have but it can be very costly. I have compiled a list of doctors (Lyme Doctors) who are knowledgeable and will have access to more accurate blood tests that could indicate whether you still have active infections. I also recommend completing the Richard Horowitz Lyme disease questionnaire which can indicate whether Lyme disease and co-infections could be a problem for you.
Next Tick Bite Prevention





